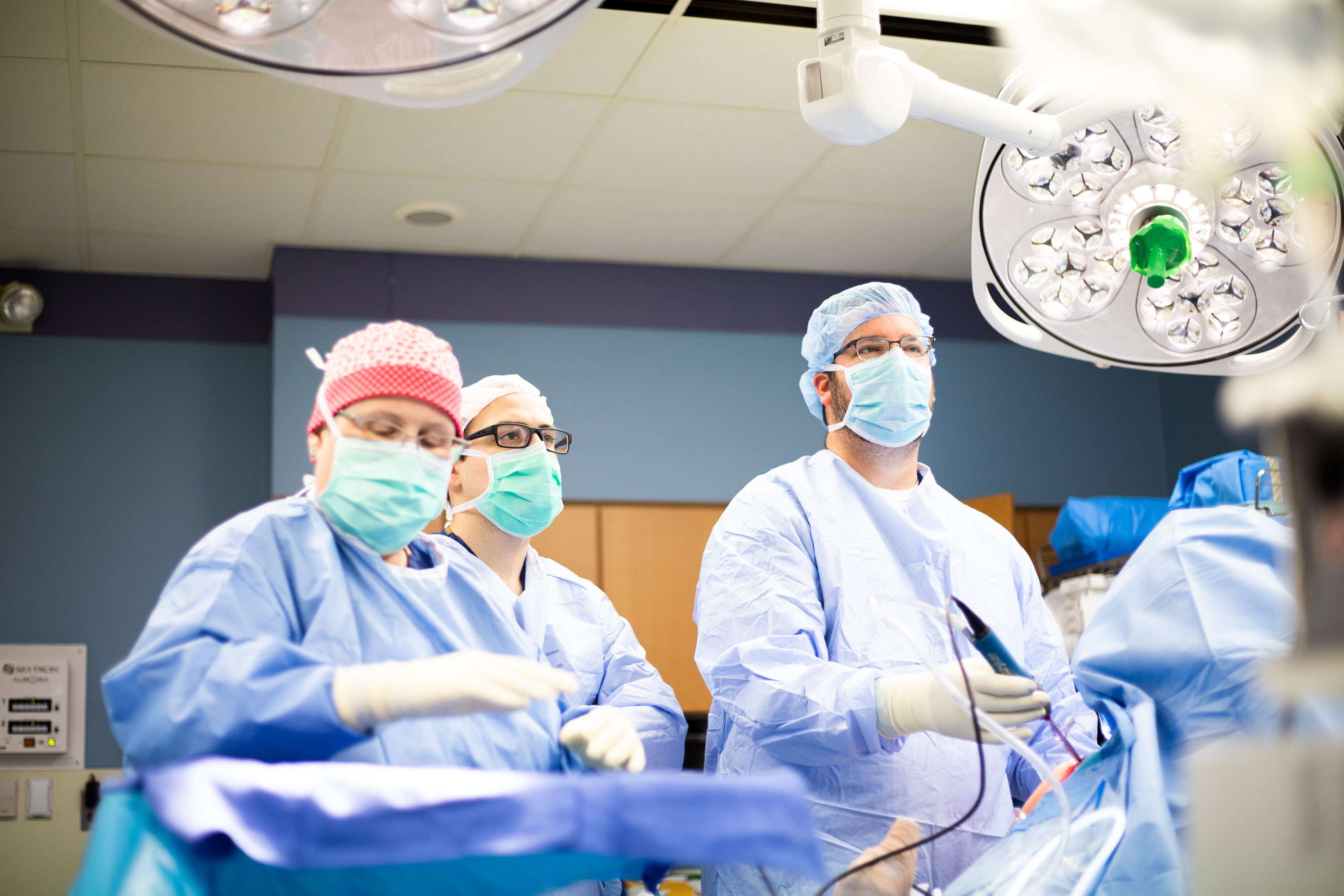
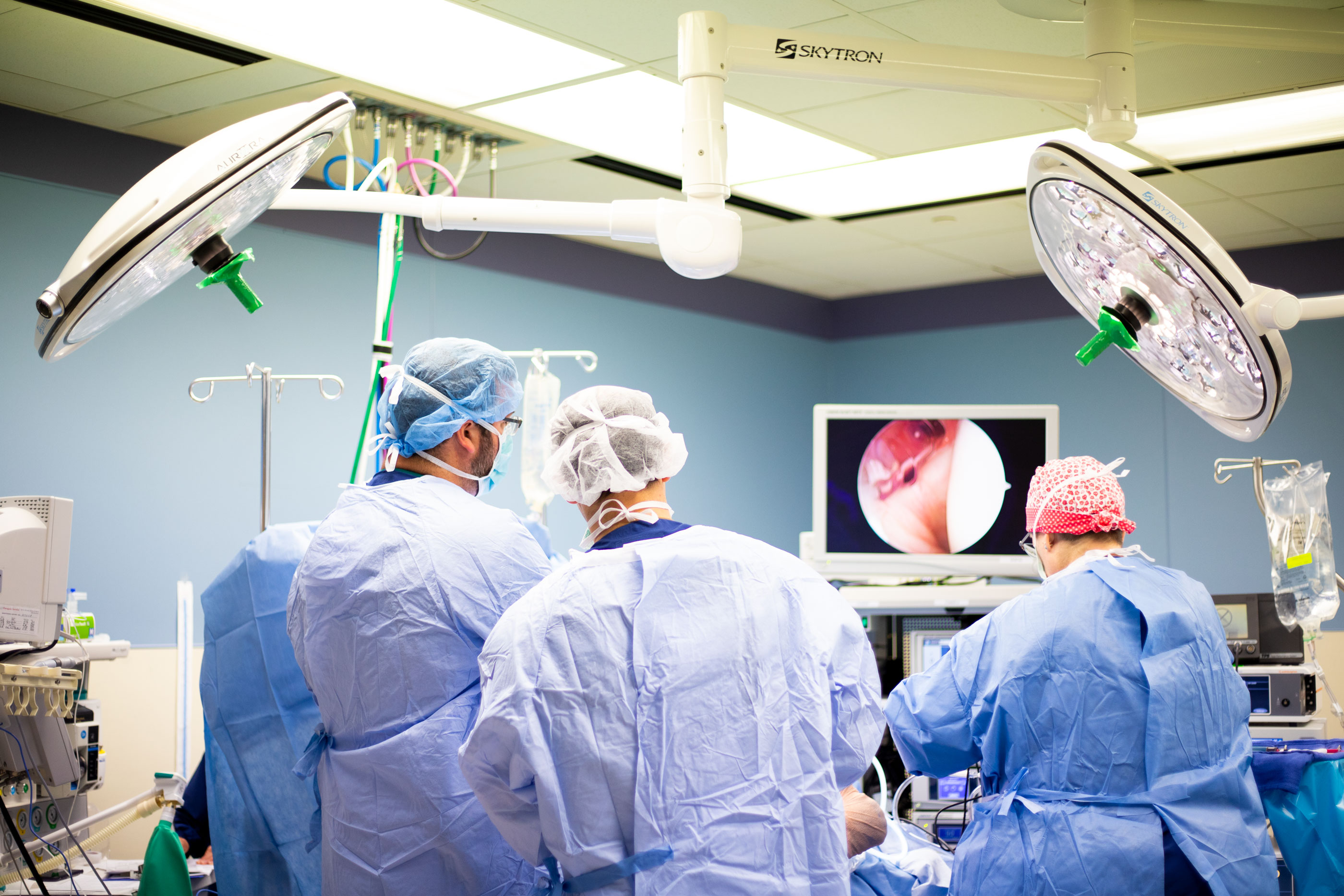
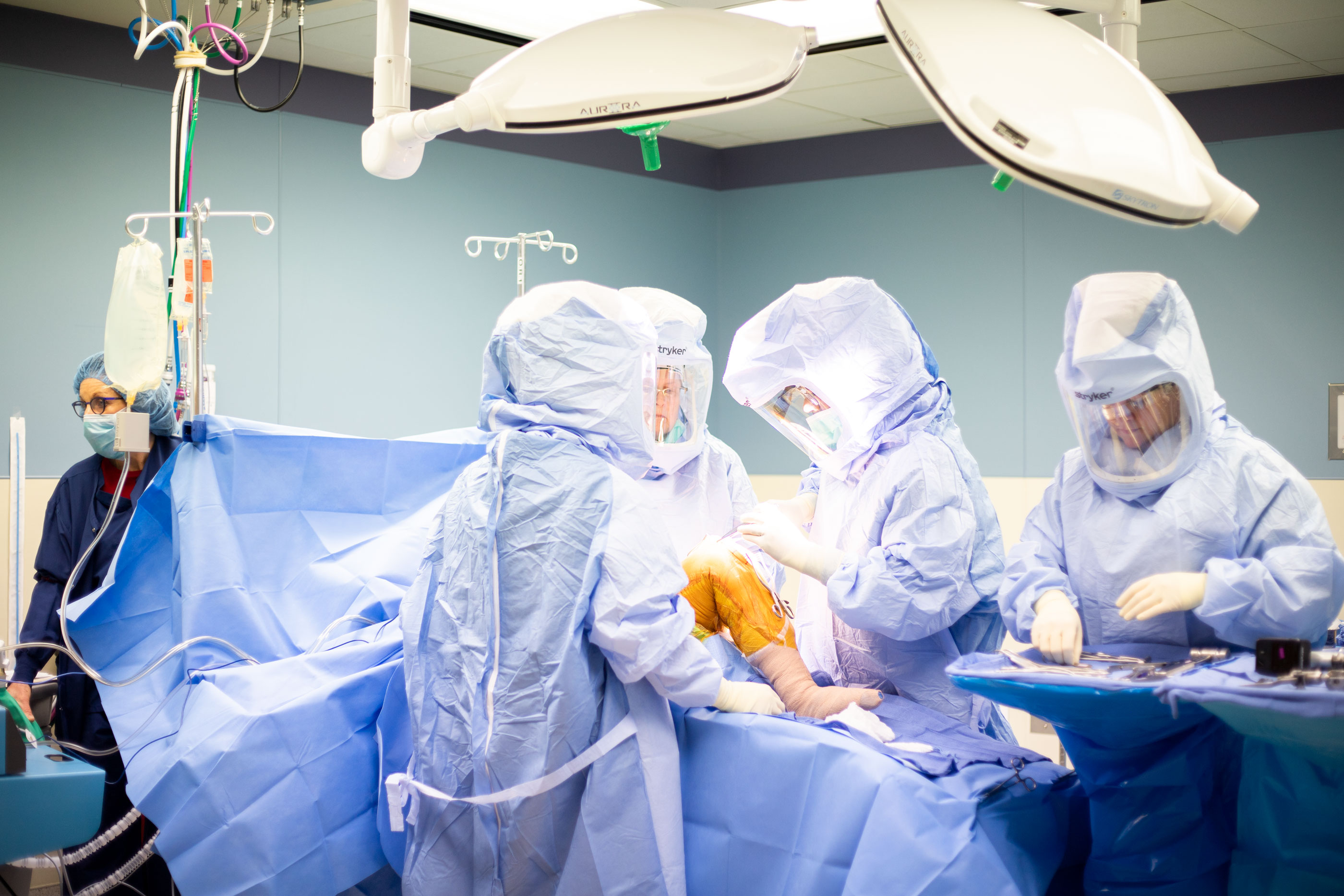
For many people, the thought of having surgery is terrifying. So, My City Wellness has “scrubbed in” with talented local surgeons as they performed a variety of procedures – a peek behind the curtain, if you will. Our sincere thanks to Ajay Srivastava, MD, Matthew Sardelli, MD and the entire team at The Surgery Center – Flint for their gracious cooperation in creating this ongoing special section.
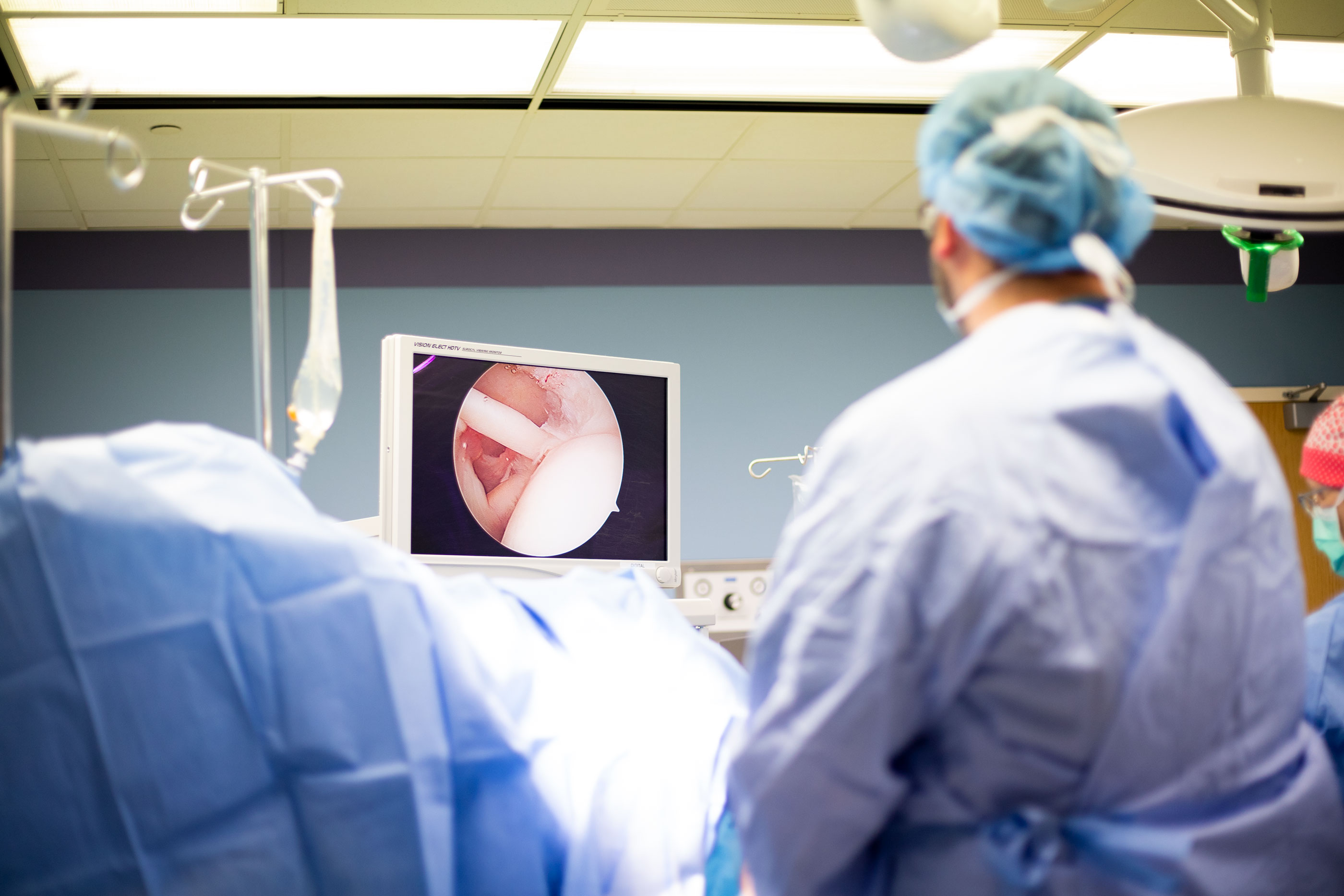
Shoulder Arthroscopy with Labral Repair
The Surgery Center – Flint
The labrum is a piece of fibrocartilage (rubbery tissue) attached to the rim of the shoulder socket that helps keep the ball of the joint in place. Surgical treatment for a shoulder labrum tear at the front of the joint is known as an arthroscopic anterior labral repair. The overall goal is to repair the torn labrum with the use of anchors attached with sutures. The anchors are first placed in the bone and then the attached sutures are passed through the torn labrum and tied down to bring the labrum back to its original attachment site on the glenoid (ring of fibrocartilage).
Labral tears may result from injury, overuse, or sometimes as part of the aging process. It causes pain and significantly limits range of motion. When a labral tear is suspected, treatment typically begins with conservative management, including physical therapy and nonsteroidal anti-inflammatory drugs. When conservative management fails, patients become candidates for arthroscopic labral repair.
The benefit of this procedure is restoration of shoulder stability and ability to resume playing sports. The arthroscopic anchors and suture-passing devices make it innovative and effective, as well as the use of regional anesthesia (nerve block).
Following surgery, ice packs are recommended to help decrease pain and swelling, with a recommended schedule of 20 minutes, three times a day. The patient will also wear a sling for six weeks, which can result in stiffness. The sling will only be removed for bathing and when sitting alone in a quiet atmosphere. It takes 3-6 months to fully recover; most will undergo 4-6 weeks of physical therapy and can expect to return to work after three months.
The success rate of the procedure is 90 percent, and Dr. Sardelli has performed it around 500 times.
 Matthew Sardelli, MD
Matthew Sardelli, MD
A native of Michigan, Dr. Sardelli specializes in orthopedic surgery and sports medicine. He earned his undergraduate degree in physiology from Michigan State University, where he also became a Certified Athletic Trainer, and received his medical degree from Wayne State University. Dr. Sardelli completed post-education with a residency at Detroit Medical Center and later the University of Utah, as well as a fellowship in orthopedic sports medicine at TRIA Orthopedic Center in Minnesota. Dr. Sardelli enjoys helping athletes of all ages and abilities return to an active lifestyle.
Affiliations: Associate Program Director, McLaren Orthopaedic Surgery Residency Program; Treasurer, Michigan Orthopaedic Society; Team Physician, Flint City Bucks; Team Orthopaedic Surgeon, Flint Firebirds
Total Knee Arthroplasty (Knee Replacement)
The Surgery Center – Flint
The goal of total knee replacement surgery is to relieve knee pain and increase knee function by resurfacing the bones that meet at the knee joint. The surgeon removes damaged portions of bone at the end of the femur (thigh bone) and top of the tibia (shin bone) and replaces them with prosthetic components.
The most significant benefit of this outpatient procedure is elimination of the need for a hospital stay for the patient, potentially reducing the risk of hospital-acquired infection. In addition, outpatient procedures are at least 30-40 percent less expensive.
Typical candidates for this surgery are experiencing daily knee pain and stiffness, have trouble with daily activities such as climbing stairs, dressing, bathing or preparing meals, and their knee frequently “gives out.” They may have tried medications, weight loss or injections without relief.
Eligibility is evaluated on an individual basis; but, in general, a person considering this procedure should be healthy without any major heart, lung or kidney disease. Not every patient can qualify for outpatient joint replacements – eligibility is determined during the pre-surgery consultation.
This procedure utilizes newer, long-acting pain medications and a nerve block to help eliminate immediate post-operative pain to the extent that the patient can get up and walk within 1-2 hours after surgery. In addition to pain medication, Accelerated Rehab Protocol helps with quick recovery.
Knee replacement done on an outpatient basis does not change final recovery time or time to return to work. In general, one can resume driving after 2-4 weeks, and resume working anywhere between four weeks to three months, depending on nature of the job. Most people need at least four weeks of outpatient physical therapy. Motivated patients can do home exercises and forego formal physical therapy sessions. There should be someone at home to help with chores for a week to ten days following surgery.
Dr. Srivastava performs more than 300 joint replacements every year. OrthoMichigan surgeons have had 100 percent success with this procedure. In general, knee replacements performed in the U.S. have a success rate of more than 90 percent.
 Ajay Srivastava, MD
Ajay Srivastava, MD
Dr. Srivastava joined OrthoMichigan in 2010. He earned his undergraduate and medical degree in India before moving to the States. His training includes a Research Fellowship in Adult Reconstruction at Scripps Clinic in San Diego, CA and Orthopedic Surgery Residency at McLaren Flint. He has a special interest in anterior hip replacement, partial and total knee replacement. Dr. Srivastava is passionate about clinical research and high-quality resident education in Flint.
Affiliations: American Association of Orthopedic Surgeons (AAOS), American Association of Hip and Knee Surgeons (AAHKS), Orthopedic Research Society (ORS), Michigan Orthopedic Society (MOS)
Photography by Kayce McClure