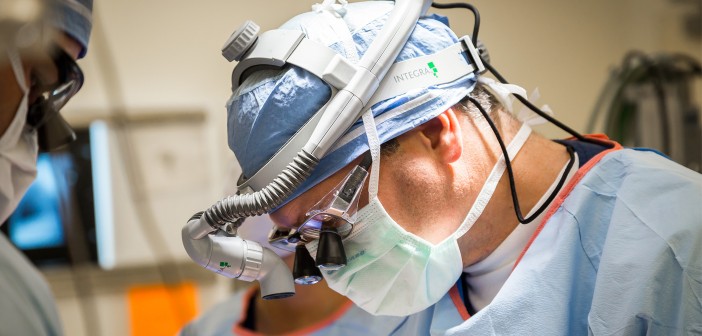
For many people, the thought of undergoing surgery is terrifying – so, My City Wellness “scrubbed in” to get up close with two talented local physicians as they performed state-of-the-art procedures. Our sincere thanks to doctors Bishr Al Dabagh, MD, FAAD and Marc Silver, MD for their gracious cooperation in creating this special section.
 Bishir Al Dabagh MD, FAAD
Bishir Al Dabagh MD, FAAD
PROCEDURE/SURGERY: Mohs Micrographic Surgery
CREDENTIALS: A board-certified dermatologist and a fellowship-trained Mohs surgeon focusing on the treatment of skin cancers, he graduated with Honors from the University of Michigan-Flint, attended medical school at Case Western Reserve University. He then trained in dermatology at Duke University and finished a Procedural Dermatology fellowship at the University of California – San Francisco.
FACILITY: Michigan Dermatology
METHOD/DESCRIPTION: This is a highly-specialized technique focusing on the accurate removal of skin cancer with margin control, while at the same time sparing the greatest amount of healthy tissue. This is accomplished by a special method of cutting the skin cancer out and then processing the tissue in a lab in the office using a unique frozen section technique while the patient waits. The surgeon reads the slides to ensure the entire cancer is removed; if not, another cut is performed (on the same day) and the tissue is tested again. The procedure is repeated until all the cancer has been removed.
The surgeon then performs reconstruction of the defect. It is an all-in-one: surgical removal, pathology and reconstruction. There is no need to go to a surgical center or hospital and the patient can go home on the same day.
This surgery is very innovative because the surgeon is also the pathologist and checks 100 percent of the margin (all the peripheral and deep margin), whereas standard excision procedures need at least two doctors (surgeon and pathologist, and in some cases, anesthesiologist) and only samples the margins instead of checking 100 percent of it. Mohs surgery has the highest cure rate of any other modality (excision, radiation, creams, curettage), with cure rates of 99 percent for primary basal cell and squamous cell carcinomas. Dr. Al Dabagh has performed this surgery 3,500 times.

The Michigan Dermatology team includes (BACK L-R) Kaylee Moyer, Megan Niezgucki, Allie Keel, Jennifer Havermale and (FRONT L-R) Hannah Scherba, Dr. Al Dabagh, Kaitlyn Scott, Donnita Edwards
The surgery is done under local anesthetic only, making it a very safe and well-tolerated procedure. The patient is awake during surgery and does not need to fast the day before. After surgery, the patient should not engage in exercise or arduous activity. They should follow their wound care instructions and follow-up with the surgeon for wound check and suture removal. Not all skin cancers are appropriate for Mohs surgery. The type, location, size and patient factors are all important.
 Marc Silver, MD, FACS
Marc Silver, MD, FACS
PROCEDURE/SURGERY: Coronary Artery Bypass
CREDENTIALS: Dual board certification – general surgery and cardiothoracic surgery
FACILITY: Genesys Heart Institute
METHOD/DESCRIPTION: The underlying condition that warrants a Coronary Artery Bypass is a blockage in the arteries around the heart that supply the blood flow, oxygen and nutrients to the muscle. When the flow is blocked and limited, heart function can diminish over time, and there is risk for a heart attack. This operation brings another source of blood flow around these blockages. Those with severe coronary artery disease benefit most from Coronary Artery Bypass. In these patients, the surgery not only improves survival, but preserves and can even improve cardiac function. The end effect is a sustained quality of life.
Coronary Artery Bypass is the most intensively studied operation in medical history. It has become a reproducible and very predictable operation that Dr. Silver has done thousands of times.
He begins by harvesting blood vessels (graft) from elsewhere in the body; often the arm, chest wall, or leg. He prepares those blood vessels to supply the heart. Then, he exposes the heart. He will typically put someone on the heart/lung machine to support blood flow during surgery. For each blocked blood vessel (graft), Dr. Silver goes beyond the blockage and attaches the harvested vessels – a “detour” around the blockage. The free end of the graft is then connected to a source of blood flow, typically the aorta. This creates the new source of blood to the heart, bypassing the blockages. The newly created blood flow will protect the heart from future heart attacks.
Overall, this surgery has 98.3-4% success rate, with of course, individual risk. It takes several weeks for the patient to feel “normal” again. In the short term, they can experience fatigue that slowly subsides. In the long run, most find that their energy level, ability to exert themselves, and functional status has improved. This is an inpatient procedure, and the patient will be in the hospital for about five days afterwards.
If a patient is considering returning to work, when they can do it will depend on the type of job: if it requires little exertion or physical activity, they can return in 4-6 weeks. For heavy physical activity, it may take 6-12 weeks. Once recovered, the patient can do everything they did prior and resume full, unrestricted activity.

(L-R) The team that performed the CABG procedure includes: Cassie Batterbee, RN; Andy Standley, PA; Candie Peake, Surgical Tech; Christine Smith, Melinda Mizikow, Surgical Tech; Keisha Redmond, Eric Leiendecker, Marc Silver, MD, FACS; James Many, Surgical Tech & Dana Shaver, RN.
Photography by Eric Dutro